Tuesday Poster Session
Category: Colon
P3115 - An Interesting Presentation of Pneumatosis coli
Tuesday, October 24, 2023
10:30 AM - 4:00 PM PT
Location: Exhibit Hall
Has Audio
- NC
Nicholas Ciurczack, DO
Valley Hospital Medical Center
Las Vegas, NV
Presenting Author(s)
John Ko, DO, Levon Tantoushian, DO, Nicholas Ciurczack, DO, Vishvinder Sharma, MD, Rebecca Salvo, DO, Scott Diamond, DO
Valley Hospital Medical Center, Las Vegas, NV
Introduction: Pneumatosis Coli is described as gas bubbles in the submucosa or subserosa of bowel wall. Etiologies in adults are broad but seen in patients presenting with COPD, bowel ischemia, on chemotherapeutic or immunosuppressive drugs, pyloric stenosis, or incidentally as a benign finding. This case is an unusual cause for pneumatosis coli.
Case Description/Methods: 50-year-old male with no significant past medical history presented to Valley Hospital for periumbilical abdominal pain and distention. He endorsed symptoms of nausea, vomiting, poor oral intake, and 25-pound weight loss. A month prior, he was diagnosed with periumbilical cellulitis and treated with clindamycin. CT abdomen/Pelvis with iv contrast showed pneumatosis coli with concerns for potential Toxic megacolon versus bowel ischemia. Infectious workup was initiated and came back positive for Clostridium Difficile. The patient denied having diarrhea and reported having normal bowel movements despite not passing gas for 2 days. He had normal vitals, white blood cell count, C-reactive protein, and lactic acid. Abdominal exam was notable for tenderness to palpation but no signs of peritonitis. CT abdominal angiography showed no evidence of ischemic bowel. Initially, he was treated conservatively with a nasogastric tube, fluids, IV flagyl, and oral vancomycin. Serial abdominal xrays were done daily to assess for free air under the diaphragm. On his third admission day, the patient developed worsening abdominal pain, peritonitis, and tachycardia. Subsequent abdominal xray demonstrated extensive pneumoperitoneum. He was taken back for an exploratory laparotomy with subtotal colectomy and end ileostomy. During the operation, there was feculent peritonitis with cecal perforation. The colon appeared healthy at the descending portion and the surgeon elected to do a flexible sigmoidoscopy and a fungating friable mass was discovered about 10 cm away from the anal verge. Multiple biopsies were taken, and a sigmoid colon mucous fistula with end ileostomy was placed. Patient was subsequently referred to Heme/Onc for further management and staging of his rectal cancer.
Discussion: There have been cases of Pneumatosis Coli mimicking colorectal cancer or resulting because of chemotherapy, but not one where pneumatosis coli was suspected to have been caused by the presence of rectal cancer. By highlighting this etiology of pneumatosis coli, providers can consider other options for causes in their differentials that are not classically highlighted.
Disclosures:
John Ko, DO, Levon Tantoushian, DO, Nicholas Ciurczack, DO, Vishvinder Sharma, MD, Rebecca Salvo, DO, Scott Diamond, DO. P3115 - An Interesting Presentation of Pneumatosis coli, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
Valley Hospital Medical Center, Las Vegas, NV
Introduction: Pneumatosis Coli is described as gas bubbles in the submucosa or subserosa of bowel wall. Etiologies in adults are broad but seen in patients presenting with COPD, bowel ischemia, on chemotherapeutic or immunosuppressive drugs, pyloric stenosis, or incidentally as a benign finding. This case is an unusual cause for pneumatosis coli.
Case Description/Methods: 50-year-old male with no significant past medical history presented to Valley Hospital for periumbilical abdominal pain and distention. He endorsed symptoms of nausea, vomiting, poor oral intake, and 25-pound weight loss. A month prior, he was diagnosed with periumbilical cellulitis and treated with clindamycin. CT abdomen/Pelvis with iv contrast showed pneumatosis coli with concerns for potential Toxic megacolon versus bowel ischemia. Infectious workup was initiated and came back positive for Clostridium Difficile. The patient denied having diarrhea and reported having normal bowel movements despite not passing gas for 2 days. He had normal vitals, white blood cell count, C-reactive protein, and lactic acid. Abdominal exam was notable for tenderness to palpation but no signs of peritonitis. CT abdominal angiography showed no evidence of ischemic bowel. Initially, he was treated conservatively with a nasogastric tube, fluids, IV flagyl, and oral vancomycin. Serial abdominal xrays were done daily to assess for free air under the diaphragm. On his third admission day, the patient developed worsening abdominal pain, peritonitis, and tachycardia. Subsequent abdominal xray demonstrated extensive pneumoperitoneum. He was taken back for an exploratory laparotomy with subtotal colectomy and end ileostomy. During the operation, there was feculent peritonitis with cecal perforation. The colon appeared healthy at the descending portion and the surgeon elected to do a flexible sigmoidoscopy and a fungating friable mass was discovered about 10 cm away from the anal verge. Multiple biopsies were taken, and a sigmoid colon mucous fistula with end ileostomy was placed. Patient was subsequently referred to Heme/Onc for further management and staging of his rectal cancer.
Discussion: There have been cases of Pneumatosis Coli mimicking colorectal cancer or resulting because of chemotherapy, but not one where pneumatosis coli was suspected to have been caused by the presence of rectal cancer. By highlighting this etiology of pneumatosis coli, providers can consider other options for causes in their differentials that are not classically highlighted.

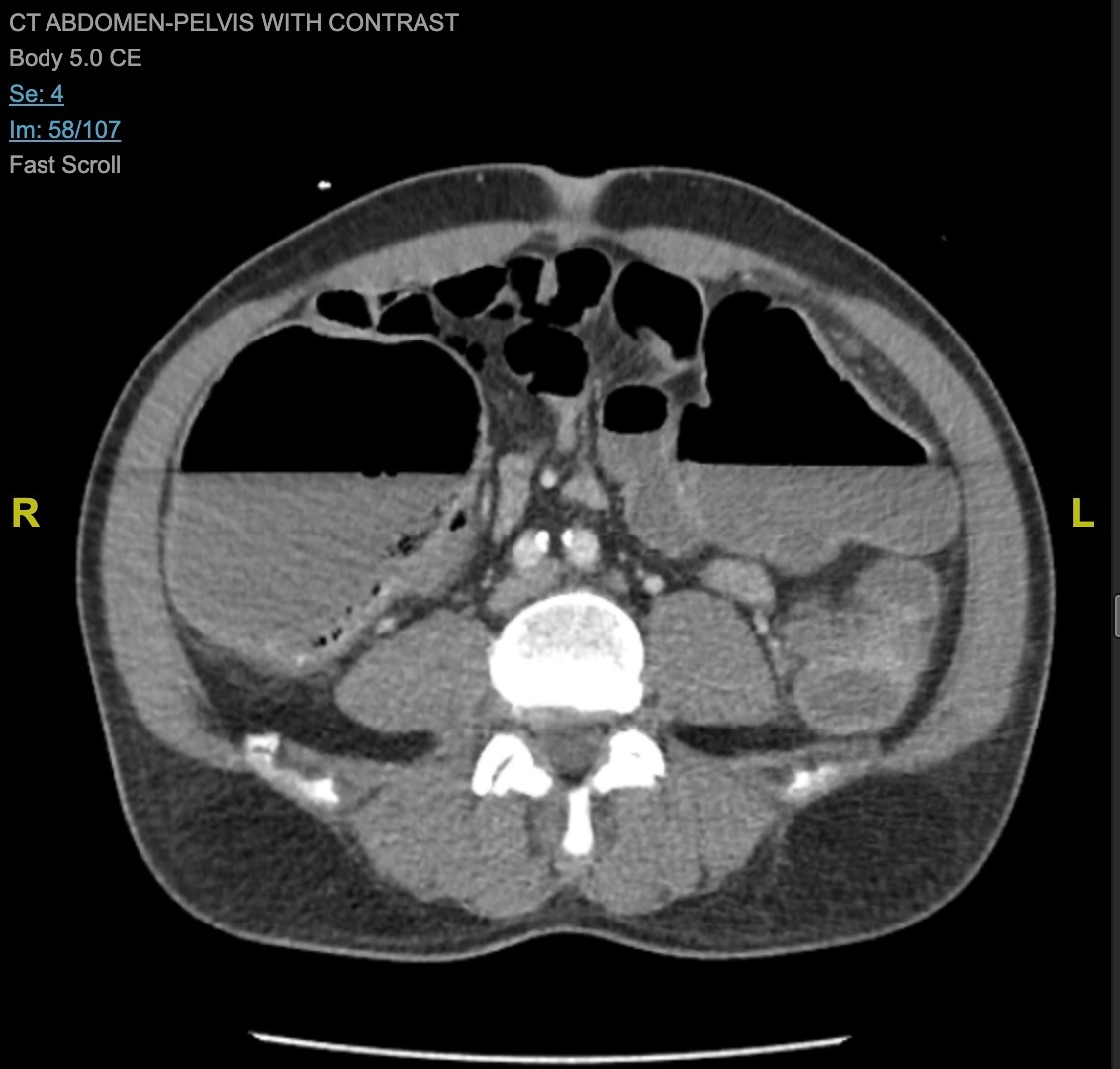
Figure: Pneumatosis intestinalis of the ascending colon
Disclosures:
John Ko indicated no relevant financial relationships.
Levon Tantoushian indicated no relevant financial relationships.
Nicholas Ciurczack indicated no relevant financial relationships.
Vishvinder Sharma indicated no relevant financial relationships.
Rebecca Salvo indicated no relevant financial relationships.
Scott Diamond indicated no relevant financial relationships.
John Ko, DO, Levon Tantoushian, DO, Nicholas Ciurczack, DO, Vishvinder Sharma, MD, Rebecca Salvo, DO, Scott Diamond, DO. P3115 - An Interesting Presentation of Pneumatosis coli, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
