Sunday Poster Session
Category: Colon
P0213 - Crossing Denonvilliers’ Fascia: Rectal Bleeding and Iron Deficiency Anemia From Prostate Cancer
Sunday, October 22, 2023
3:30 PM - 7:00 PM PT
Location: Exhibit Hall
Has Audio

Kwabena O. Adu-Gyamfi, MD
Medical College of Georgia at Augusta University
Augusta, GA
Presenting Author(s)
Kwabena O. Adu-Gyamfi, MD1, Dhanush Shimoga, MBBS2, Praneeth Kudaravalli, MD3, Angela Barnes, MD2, Amanda Barrett, MD2, Amol Sharma, MD, MS, FACG2
1Medical College of Georgia at Augusta University, Augusta, GA; 2Medical College of Georgia at Augusta University, Augusta, GA; 3Augusta University, Augusta, GA
Introduction: Prostate cancer involving the rectal mucosa is rare despite the anatomic proximity of the two structures. The majority of case reports are found in the radiology and pathology literature. The most common clinical presentation of prostate cancer in the rectum is perineal pain. We present a case of a middle-aged man with prostate cancer who presented for outpatient colonoscopy for intermittent rectal bleeding and iron deficiency anemia.
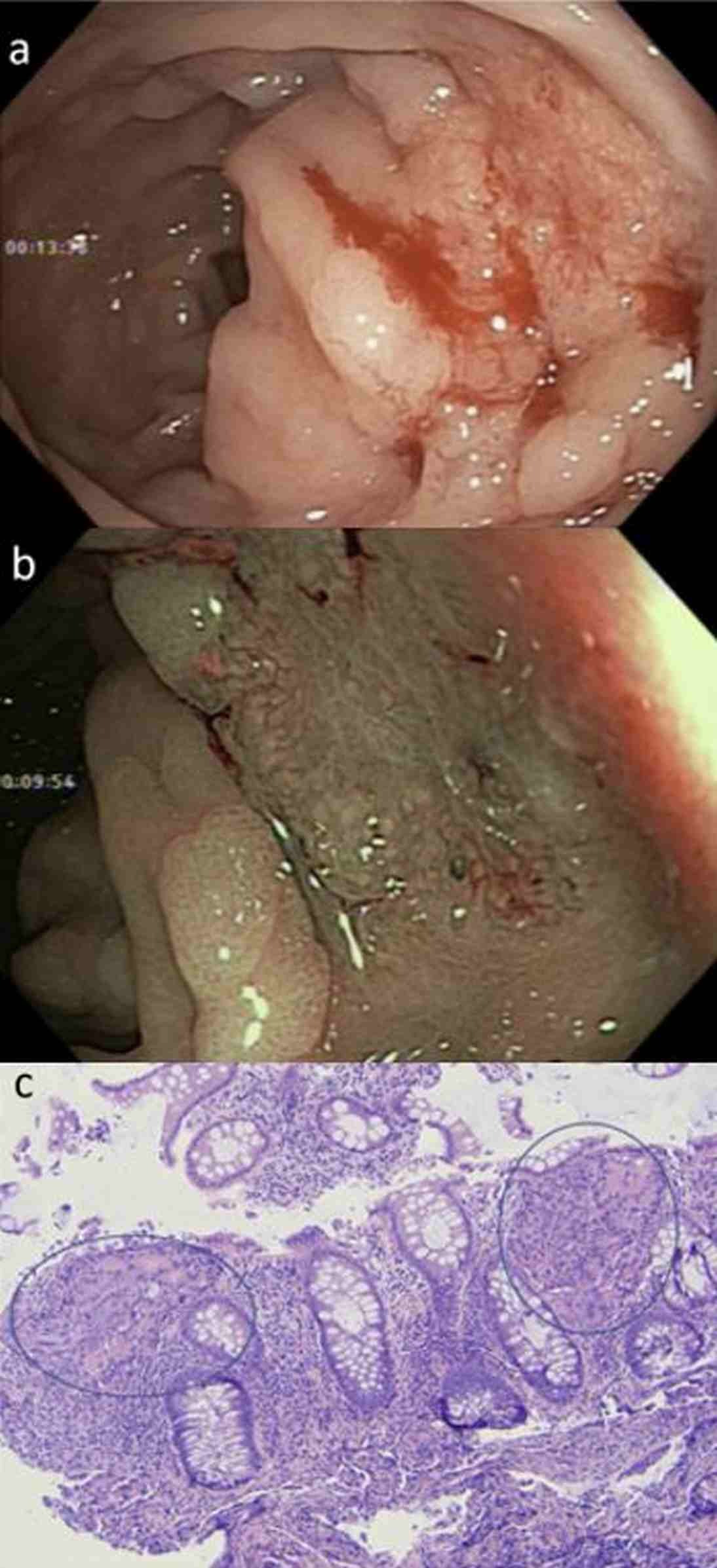
Case Description/Methods: A 59-year-old Caucasian man with history of castration-resistant prostate cancer with bone and liver metastasis after chemoradiation therapy and immunotherapy developed iron deficiency anemia and intermittent rectal bleeding. He attributed his rectal bleeding to internal hemorrhoids. During an outpatient colonoscopy, a flat dysplastic-appearing 15mm lesion was seen in the proximal anterolateral rectum (Fig 1a) and non-bleeding Grade I internal hemorrhoids. Narrow-band imaging (NBI) revealed central scarring of the lesion (Fig 1b). Histopathology of lesion biopsies revealed islands of infiltrating carcinoma between normal colonic glands (Fig 1c). Immunohistochemical staining was positive for NKX3.1 and negative for CDX-2 consistent with prostate cancer involving the rectal wall. He opted for palliative care and passed away peacefully four months later.
Discussion: Prostate cancer involving the rectal wall may occur through hematogenous, lymphatic or by contiguous spread. Contiguous spread to the rectum is rare because of the thick fibrous Denonvilliers’ (rectoprostatic) fascia posterior to the prostate gland. Affected patients commonly present with perineal pain. Our patient presented with rectal bleeding and iron deficiency anemia, for which the differential diagnosis includes other anorectal pathology such as hemorrhoids or radiation proctopathy. Lesions in early stages may be subtle requiring careful endoscopic examination for detection and may also mimic primary rectal adenocarcinoma both endoscopically and histologically. This has led to a misdiagnosis in some published cases. Compatible histology and staining clinched the diagnosis in our case. The 5-year overall survival of patients with prostate cancer involving the rectum is less than 40%. Prior hormonal therapy and rectal bleeding are associated with increased mortality. A high index of suspicion and increased recognition of this phenomenon by gastroenterologists will help prevent diagnostic pitfalls and provide accurate information to patients during multidisciplinary care.
Disclosures:
Kwabena O. Adu-Gyamfi, MD1, Dhanush Shimoga, MBBS2, Praneeth Kudaravalli, MD3, Angela Barnes, MD2, Amanda Barrett, MD2, Amol Sharma, MD, MS, FACG2. P0213 - Crossing Denonvilliers’ Fascia: Rectal Bleeding and Iron Deficiency Anemia From Prostate Cancer, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
1Medical College of Georgia at Augusta University, Augusta, GA; 2Medical College of Georgia at Augusta University, Augusta, GA; 3Augusta University, Augusta, GA
Introduction: Prostate cancer involving the rectal mucosa is rare despite the anatomic proximity of the two structures. The majority of case reports are found in the radiology and pathology literature. The most common clinical presentation of prostate cancer in the rectum is perineal pain. We present a case of a middle-aged man with prostate cancer who presented for outpatient colonoscopy for intermittent rectal bleeding and iron deficiency anemia.
Case Description/Methods: A 59-year-old Caucasian man with history of castration-resistant prostate cancer with bone and liver metastasis after chemoradiation therapy and immunotherapy developed iron deficiency anemia and intermittent rectal bleeding. He attributed his rectal bleeding to internal hemorrhoids. During an outpatient colonoscopy, a flat dysplastic-appearing 15mm lesion was seen in the proximal anterolateral rectum (Fig 1a) and non-bleeding Grade I internal hemorrhoids. Narrow-band imaging (NBI) revealed central scarring of the lesion (Fig 1b). Histopathology of lesion biopsies revealed islands of infiltrating carcinoma between normal colonic glands (Fig 1c). Immunohistochemical staining was positive for NKX3.1 and negative for CDX-2 consistent with prostate cancer involving the rectal wall. He opted for palliative care and passed away peacefully four months later.
Discussion: Prostate cancer involving the rectal wall may occur through hematogenous, lymphatic or by contiguous spread. Contiguous spread to the rectum is rare because of the thick fibrous Denonvilliers’ (rectoprostatic) fascia posterior to the prostate gland. Affected patients commonly present with perineal pain. Our patient presented with rectal bleeding and iron deficiency anemia, for which the differential diagnosis includes other anorectal pathology such as hemorrhoids or radiation proctopathy. Lesions in early stages may be subtle requiring careful endoscopic examination for detection and may also mimic primary rectal adenocarcinoma both endoscopically and histologically. This has led to a misdiagnosis in some published cases. Compatible histology and staining clinched the diagnosis in our case. The 5-year overall survival of patients with prostate cancer involving the rectum is less than 40%. Prior hormonal therapy and rectal bleeding are associated with increased mortality. A high index of suspicion and increased recognition of this phenomenon by gastroenterologists will help prevent diagnostic pitfalls and provide accurate information to patients during multidisciplinary care.

Figure: Fig 1a. Endoscopic picture showing rectal mucosal involvement of prostate cancer. Fig 1b. Endoscopic picture showing rectal lesion in narrow band imaging (NBI). Fig 1c. Histology slide 100x H&E: Islands of infiltrating prostate adenocarcinoma (circled) appear between normal colonic glands.
Disclosures:
Kwabena Adu-Gyamfi indicated no relevant financial relationships.
Dhanush Shimoga indicated no relevant financial relationships.
Praneeth Kudaravalli indicated no relevant financial relationships.
Angela Barnes indicated no relevant financial relationships.
Amanda Barrett indicated no relevant financial relationships.
Amol Sharma indicated no relevant financial relationships.
Kwabena O. Adu-Gyamfi, MD1, Dhanush Shimoga, MBBS2, Praneeth Kudaravalli, MD3, Angela Barnes, MD2, Amanda Barrett, MD2, Amol Sharma, MD, MS, FACG2. P0213 - Crossing Denonvilliers’ Fascia: Rectal Bleeding and Iron Deficiency Anemia From Prostate Cancer, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
