Sunday Poster Session
Category: IBD
P0824 - Concomitant Crohn's Disease and Hidradenitis Suppurativa With Severe Stricturing Peri-Anal Disease
Sunday, October 22, 2023
3:30 PM - 7:00 PM PT
Location: Exhibit Hall
Has Audio
- DC
David L. Cheung, MD
UC Irvine
Orange, CA
Presenting Author(s)
David L. Cheung, MD1, Amirali Tavangar, MD2, Andy Lin, MD2, Neil Jariwalla, MD2, Peter Nguyen, MD2, Joshua Kwon, MD2, Jason Samarasena, MD2
1UC Irvine, Orange, CA; 2University of California Irvine, Orange, CA
Introduction: Crohn’s disease (CD) is an inflammatory bowel disease that presents with both intestinal and extraintestinal manifestations. While a clinically different presentation, Hidradenitis Suppurativa (HS) shares CD’s inflammatory presentation, forming debilitating sterile skin abscesses, scarring, sinus tracts, perianal fistulas, and stenosis. This case describes a case of active Crohn's flare, but with extensive history of HS, obfuscating the clear etiology of the patient’s anocutaneous fistulas and acute on chronic anal stenosis.
Case Description/Methods: A 43-year-old male, with a history of tobacco use, recently diagnosed CD and longstanding pelvic HS, presents with perirectal drainage and anal stenosis (Image A/B). Initial CT imaging showed anocutaneous fistulas extending into the bilateral gluteal skin surfaces, circumferential mural thickening from anus to descending colon, and perineal, gluteal, and thigh HS (Image C). The patient reported poor compliance with his mesalamine therapy but reported relatively good control of his pelvic HS up until this point, which had previously undergone debridement, skin grafting/flaps, and diverting colostomy with anoplasty. Colonoscopy revealed significant anal stenosis within the gluteal folds from previous HS interventions, a stenotic bowel lumen 25 cm from the anus that was un-advanceable, and circumferential inflammation and deep ulcerations within the rectum (Image D). Biopsy revealed severe active chronic colitis consistent with Crohn’s flare. The patient was subsequently started on a prednisone taper with the intention to follow up for anti-TNF alpha therapy.
Discussion: While no clear correlation between CD and HS has been clearly established, recent studies have suggested an association between the two disease processes. Both diseases have been associated with elevated inflammatory factors, such as IL-1, IL-6, IL-17, IL-23, and TNF, hence the use of biologics in the treatment of severe stages of both diseases. Patients with IBD also have a 9 times increased risk of developing HS compared to the general population. Despite prior well managed HS, a flare of the patient’s CD led to formation of anocutaneous fistulas and exacerbation of existing anal stenosis. This case highlights the interconnected prevalence and possible synergistic effect of the two diseases in the setting of perianal disease. The presence of gastrointestinal symptoms and concomitant HS perianal disease should prompt colonoscopy evaluation for a potential Crohn’s flare.
Disclosures:
David L. Cheung, MD1, Amirali Tavangar, MD2, Andy Lin, MD2, Neil Jariwalla, MD2, Peter Nguyen, MD2, Joshua Kwon, MD2, Jason Samarasena, MD2. P0824 - Concomitant Crohn's Disease and Hidradenitis Suppurativa With Severe Stricturing Peri-Anal Disease, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
1UC Irvine, Orange, CA; 2University of California Irvine, Orange, CA
Introduction: Crohn’s disease (CD) is an inflammatory bowel disease that presents with both intestinal and extraintestinal manifestations. While a clinically different presentation, Hidradenitis Suppurativa (HS) shares CD’s inflammatory presentation, forming debilitating sterile skin abscesses, scarring, sinus tracts, perianal fistulas, and stenosis. This case describes a case of active Crohn's flare, but with extensive history of HS, obfuscating the clear etiology of the patient’s anocutaneous fistulas and acute on chronic anal stenosis.
Case Description/Methods: A 43-year-old male, with a history of tobacco use, recently diagnosed CD and longstanding pelvic HS, presents with perirectal drainage and anal stenosis (Image A/B). Initial CT imaging showed anocutaneous fistulas extending into the bilateral gluteal skin surfaces, circumferential mural thickening from anus to descending colon, and perineal, gluteal, and thigh HS (Image C). The patient reported poor compliance with his mesalamine therapy but reported relatively good control of his pelvic HS up until this point, which had previously undergone debridement, skin grafting/flaps, and diverting colostomy with anoplasty. Colonoscopy revealed significant anal stenosis within the gluteal folds from previous HS interventions, a stenotic bowel lumen 25 cm from the anus that was un-advanceable, and circumferential inflammation and deep ulcerations within the rectum (Image D). Biopsy revealed severe active chronic colitis consistent with Crohn’s flare. The patient was subsequently started on a prednisone taper with the intention to follow up for anti-TNF alpha therapy.
Discussion: While no clear correlation between CD and HS has been clearly established, recent studies have suggested an association between the two disease processes. Both diseases have been associated with elevated inflammatory factors, such as IL-1, IL-6, IL-17, IL-23, and TNF, hence the use of biologics in the treatment of severe stages of both diseases. Patients with IBD also have a 9 times increased risk of developing HS compared to the general population. Despite prior well managed HS, a flare of the patient’s CD led to formation of anocutaneous fistulas and exacerbation of existing anal stenosis. This case highlights the interconnected prevalence and possible synergistic effect of the two diseases in the setting of perianal disease. The presence of gastrointestinal symptoms and concomitant HS perianal disease should prompt colonoscopy evaluation for a potential Crohn’s flare.

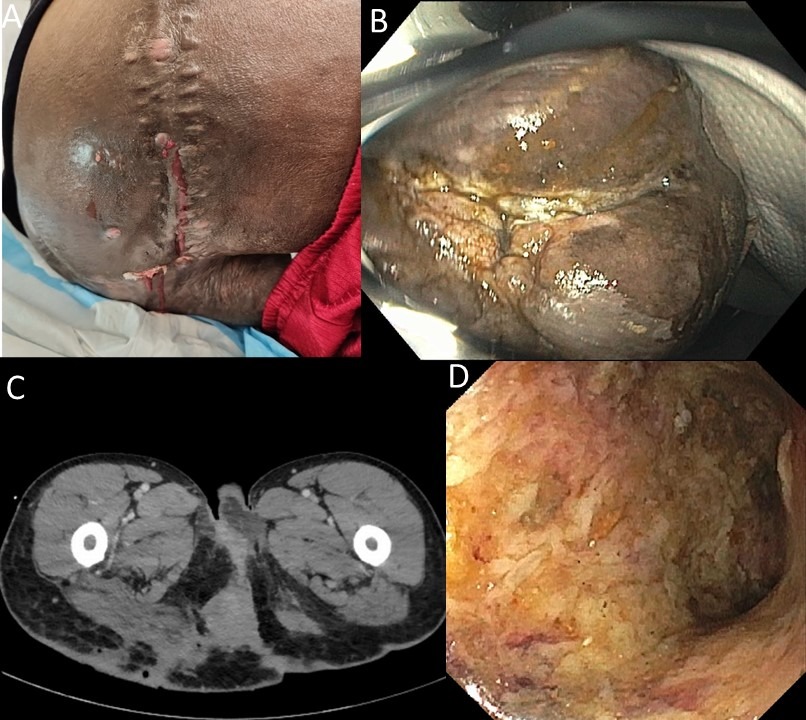
Figure: A) Severe hidradenitis suppurative involving perineum, bilateral gluteal and upper superior right thigh soft tissues and bilateral complex anocutaneous fistulas of the right and left gluteal skin surfaces
B) Gross anal stenosis present on colonoscopic evaluation
C) CT abdomen and pelvis with evidence of severe HS and anocutaneous fistulas
D) Colonoscopic evaluation with circumferential deep ulceration at the rectum with stenotic bowel 25 cm from the anus
B) Gross anal stenosis present on colonoscopic evaluation
C) CT abdomen and pelvis with evidence of severe HS and anocutaneous fistulas
D) Colonoscopic evaluation with circumferential deep ulceration at the rectum with stenotic bowel 25 cm from the anus
Disclosures:
David Cheung indicated no relevant financial relationships.
Amirali Tavangar indicated no relevant financial relationships.
Andy Lin indicated no relevant financial relationships.
Neil Jariwalla indicated no relevant financial relationships.
Peter Nguyen indicated no relevant financial relationships.
Joshua Kwon indicated no relevant financial relationships.
Jason Samarasena: Applied Medical – Advisor or Review Panel Member. Boston Scientific – Consultant. Conmed – Consultant. Cook – Educational Grant. Neptune Medical – Consultant. Olympus – Consultant. Steris – Consultant.
David L. Cheung, MD1, Amirali Tavangar, MD2, Andy Lin, MD2, Neil Jariwalla, MD2, Peter Nguyen, MD2, Joshua Kwon, MD2, Jason Samarasena, MD2. P0824 - Concomitant Crohn's Disease and Hidradenitis Suppurativa With Severe Stricturing Peri-Anal Disease, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
