Back

Sunday Poster Session
Category: Liver
P1026 - PSC in an Acutely Psychotic Patient
Sunday, October 22, 2023
3:30 PM – 7:00 PM PT
Location: Exhibit Hall

Has Audio

Andrea R. Amaro, MD
University of Texas Southwestern Medical Center
Dallas, TX
Presenting Author(s)
Andrea R.. Amaro, MD1, Justin Brewer, PA-C2, Neeraj K. Kalra, MD3
1University of Texas Southwestern Medical Center, Dallas, TX; 2Parkland Health, Carrollton, TX; 3University of Texas Southwestern Medical Center, Southlake, TX
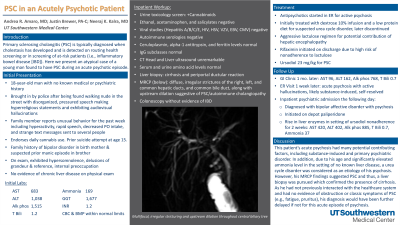
Introduction: Primary sclerosing cholangitis (PSC) is typically diagnosed when cholestasis has developed and is detected on routing health screening or in screening of at-risk patients (i.e., inflammatory bowel disease [IBD]). Here we present an atypical case of a young man found to have PSC during an acute psychotic episode.
Case Description/Methods: An 18-year-old man with no prior medical or psychiatric history presented under involuntary custody after being found walking publicly in the nude. He exhibited disorganized, pressured speech, hyperreligious delusions, and audiovisual hallucinations. He had a family history of bipolar I disorder. He was found to have elevated liver enzymes—AST 301, ALT 327, Alk phos 862, GGT 1677, total bilirubin 0.8, INR 1.3, ammonia 169—without asterixis or stigmata of chronic liver disease on exam. His MELD-Na was 10, albumin 4.9, platelets 357. Urine toxicology was positive for cannabis. Ethanol, acetaminophen, and salicylate levels were negative. Viral and autoimmune serologies were negative. Ceruloplasmin, alpha-1 antitrypsin, ferritin, and IgG subclasses were normal. CT head and liver ultrasound were unremarkable. He was given antipsychotics, a dextrose infusion and low protein diet for suspected urea cycle disorder, and lactulose and rifaximin for hepatic encephalopathy. Ammonia levels were monitored daily as a rise above 200 would require renal replacement therapy to prevent cerebral edema. Serum and urine amino acid levels later returned normal. A liver biopsy was obtained which showed bridging and septal fibrosis with nodule formation, consistent with cirrhosis, along with periportal ductular reaction. MRCP showed irregular strictures with upstream biliary dilation, diffuse wall thickening and enhancement of the right, left and common hepatic ducts and common bile duct, suggestive of primary sclerosing cholangitis. He was started on ursodiol and underwent colonoscopy without evidence of IBD.
Discussion: This patient had many potential contributors to his psychosis, including substance-induced, primary psychiatric disease, and metabolic encephalopathy from high ammonia. Lack of classic symptoms (e.g., fatigue, pruritus) and an unremarkable preliminary workup made the diagnosis of PSC challenging. Urea cycle disorders were considered given he had no sonographic evidence of cirrhosis. Ultimately, MRCP was needed to solidify the diagnosis. While an uncommon manifestation of hepatic encephalopathy, psychosis in this case led to the discovery of PSC.
Disclosures:
Andrea R.. Amaro, MD1, Justin Brewer, PA-C2, Neeraj K. Kalra, MD3. P1026 - PSC in an Acutely Psychotic Patient, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
1University of Texas Southwestern Medical Center, Dallas, TX; 2Parkland Health, Carrollton, TX; 3University of Texas Southwestern Medical Center, Southlake, TX
Introduction: Primary sclerosing cholangitis (PSC) is typically diagnosed when cholestasis has developed and is detected on routing health screening or in screening of at-risk patients (i.e., inflammatory bowel disease [IBD]). Here we present an atypical case of a young man found to have PSC during an acute psychotic episode.
Case Description/Methods: An 18-year-old man with no prior medical or psychiatric history presented under involuntary custody after being found walking publicly in the nude. He exhibited disorganized, pressured speech, hyperreligious delusions, and audiovisual hallucinations. He had a family history of bipolar I disorder. He was found to have elevated liver enzymes—AST 301, ALT 327, Alk phos 862, GGT 1677, total bilirubin 0.8, INR 1.3, ammonia 169—without asterixis or stigmata of chronic liver disease on exam. His MELD-Na was 10, albumin 4.9, platelets 357. Urine toxicology was positive for cannabis. Ethanol, acetaminophen, and salicylate levels were negative. Viral and autoimmune serologies were negative. Ceruloplasmin, alpha-1 antitrypsin, ferritin, and IgG subclasses were normal. CT head and liver ultrasound were unremarkable. He was given antipsychotics, a dextrose infusion and low protein diet for suspected urea cycle disorder, and lactulose and rifaximin for hepatic encephalopathy. Ammonia levels were monitored daily as a rise above 200 would require renal replacement therapy to prevent cerebral edema. Serum and urine amino acid levels later returned normal. A liver biopsy was obtained which showed bridging and septal fibrosis with nodule formation, consistent with cirrhosis, along with periportal ductular reaction. MRCP showed irregular strictures with upstream biliary dilation, diffuse wall thickening and enhancement of the right, left and common hepatic ducts and common bile duct, suggestive of primary sclerosing cholangitis. He was started on ursodiol and underwent colonoscopy without evidence of IBD.
Discussion: This patient had many potential contributors to his psychosis, including substance-induced, primary psychiatric disease, and metabolic encephalopathy from high ammonia. Lack of classic symptoms (e.g., fatigue, pruritus) and an unremarkable preliminary workup made the diagnosis of PSC challenging. Urea cycle disorders were considered given he had no sonographic evidence of cirrhosis. Ultimately, MRCP was needed to solidify the diagnosis. While an uncommon manifestation of hepatic encephalopathy, psychosis in this case led to the discovery of PSC.
Disclosures:
Andrea Amaro indicated no relevant financial relationships.
Justin Brewer indicated no relevant financial relationships.
Neeraj Kalra indicated no relevant financial relationships.
Andrea R.. Amaro, MD1, Justin Brewer, PA-C2, Neeraj K. Kalra, MD3. P1026 - PSC in an Acutely Psychotic Patient, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
